Pandemics - There is no ‘normal’ to go back to
Update 30/05/2023: For practical reasons, I do not normally go back to previous posts, especially not when evolving events are concerned. Evolving knowledge and facts are part of the nature of reporting, as they are a part of your own opinions and ideas. However, in this case I felt compelled to add a few words, to make sure that the premise of this article does not leave you with a misleading impression. At the time of writing, it seems at the very least equally plausible that COVID-19 was not, in fact, of a zoonotic origin, but rather the result of a laboratory leak in the Wuhan Institute for Virology. Countries like the U.S. and China have been conducting ‘gain-of-function’ research in labs like these, in which they experiment with viruses, by for instance making them more infectious, ostensibly to learn more about how to counter them. Officials have tried to hide, lie about, or otherwise obfuscate that this research even took place there, even going so far as to make sure that scientists came out against the lab leak origin and in favour of a zoonotic origin story, and media platforms made sure that those kinds of stories were suppressed or labelled as ‘fake news’. While the information contained within this article about zoonotic diseases and other drivers of pandemics is still valid, and remain areas of concern, I did not want this article to leave you with the impression that COVID-19 was of natural origin when it appears that this is not so.
Update 05/07/2023: After doing some more research into the sequence of events surround the COVID-19 origins debate, as well as the claims made by the different scientists involved, I have changed the “it seems likely that COVID-19 was not, in fact, of a zoonotic origin…” sentence in the above update to “at the very least equally plausible”, since I could not conclusively verify the likelihood of it being either natural or man-made. This underscores the immense complexity of the virology field as well as the need for nuance in this still ongoing and highly controversial discussion.
Now that COVID-19 vaccination rates are steadily climbing, falling infection and hospitalisation rates are leading Western countries like the Netherlands to open up their societies. As schools reopen for the final weeks of the school year – even with a significant percentage of teachers still unvaccinated – and people flock to terraces and Ikea’s en masse, the situation in countries like Haiti and India is remains out of control. With much of the Global South struggling to get access to vaccines, people in India are having to resort to burning the remains of their loved ones in the street or placing them in the Ganges river, due to overflowing morgues and skyrocketing funeral costs. Who knows where we will be a couple of months from now. Maybe the vaccines will cause a decisive turning point and stop the incessant rise of the number of infections in the Global South. Or maybe the virus mutates into some vaccine-resistant strain, and we are all right back to where we were in March last year.
If there is one thing I have noticed during these long months, especially from working in secondary schools with constantly shifting schedules, lockdowns and reopenings and lockdowns and reopenings, is that people are tired. Of all of it. The health measures and vigilance for symptoms, the giving up of freedoms, the constant back and forths in measures taken to combat the virus, and the never-ending stream of conflicting news and updates. The limit of what can reasonably be expected from people has been reached if not long been surpassed.
However, this pervading feeling of finally ‘going back to normal’, despite being completely understandable, is not going to get us out of this. Don’t get me wrong, it would be a wonderful thing to once again be able to see and hug one's loved ones, to go out for dinner or drinks, and attend live music concerts. Anything beats staring at your screen for the countless online meetings that barely pass for human contact, and idly studying the same four white walls in the vain hope of deriving some sense of meaning from the patterns in the wallpaper. Instead, what I’m referring to has more to do with how we actually got into this situation, and how we are almost certain to be right back here–or in an infinitely worse situation – if we do not make some meaningful changes to the way we live and treat the world around us.
Let me briefly explain what I mean before going more in-depth. Through our actions, we are contributing to the rise of diseases and therefore increasing the risk of epidemics and pandemics (terms that are derived from ancient Greek, ‘epi’ meaning upon/among, ‘pan’ meaning all, and ‘demic’ derived from “demos”, which means people). The primary drivers are deforestation, agriculture and livestock production, climate change, wildlife exploitation and trade, and antibiotic resistance. Furthermore, travel, transport, and urbanisation make outbreaks spread around the globe with lightning speed. Over the course of this article, I want to explore and elaborate on some of the main causes, although I highly recommend you to do your own research on what is a rather complicated issue.
What are zoonotic diseases?
Before we start talking about the drivers of disease outbreaks, we should first understand what exactly we are dealing with. A term you might never have heard before the outbreak of COVID-19 (or ever) is ‘zoonotic disease’, or zoonosis. This admittedly ambiguous term refers to “any disease or infection that is naturally transmissible from vertebrate animals to humans.” In other words, diseases we can catch from (most) other animals. Think of diseases like rabies, which you could catch if you get bitten by a rabid dog, bat, or raccoon. The HIV virus is also an example of a zoonotic disease, albeit one that has mutated so that it can now only be transmitted between humans. So why is this relevant when we talk about COVID-19 and the causes of pandemics?
Well, first of all, zoonoses are the most prevalent type of diseases that form a danger to humans. At least 61% of all human pathogens are zoonotic, and have represented 75% of all emerging pathogens during the past decade. They should therefore be one of our main areas of concern if we want to prevent future pandemics. Another type of disease is the ‘vector-borne disease’, which is spread via invertibrate animals like mosquitoes, ticks, and fleas. Vector-borne diseases account for 17% of all infectious diseases. I will mainly focus on zoonotic diseases, since they are responsible for the overwhelming majority of new disease outbreaks, but will mention vector-borne diseases later on when relevant.
Disease outbreaks are on the rise
None of this is new, there have been many outbreaks of these diseases in the past. The problem, as mentioned earlier, is that the rate of these outbreaks has been increasing. Around 72% of these outbreaks have originated in wildlife with domesticated animals being the intermediary through which the diseases are passed onto humans.

Let’s take a look in some more detail at some of these outbreaks. I have to admit, in a way listing the pandemics and near-pandemics of the past two decades feels similar to listing each year’s record-breaking temperatures, since it is hard to escape the feeling that something is deeply, deeply wrong.
-In 2002-2003 there was the outbreak SARS and the bird flu H5N1 (first detected in 1997).
-In 2009 a new strain of swine flu (H1N1) emerged that infected over 760 million people and left around 284,000 people and infinitely more pigs dead. It now circulates each year.
-In 2012 the Middle East Respiratory Syndrome, or MERS, was detected, which has seen repeated surges in cases every year since, with the largest known outbreak occurring in South-Korea in 2015.
-In 2013 saw an outbreak of another strain of bird flu (H7N9). China is currently experiencing its sixth epidemic of this strain.
-The years 2014-2016 saw “the largest and most complex Ebola outbreak since the virus was first discovered in 1976”.
-In 2015 the Zika virus (a vector-borne disease, first detected in 1947) caused alarm when it infected thousands of babies and caused them to have smaller heads.
It is difficult to find a comprehensive disease outbreak list, since these diseases often mutate and then later resurface in a different forms, so I have combined several pages from the website of the U.S. Centers for Disease Control and Prevention, the UNEP Frontiers 2016 report mentioned several times throughout this article, in addition to one summarising article from the Independent to compile this list, which should not be interpreted as a comprehensive or completely accurate overview but more as an indication.
So how does COVID-19 compare to these outbreaks? Well, the number of infections is relatively high – though not the highest – and still rising. At the time of writing ~180 million have been infected worldwide. This disease’s infectiousness is one of the main reasons why the death toll is so high, even though its mortality rate is probably in the range of one or two percent (higher estimates often go up to around five or six percent). It should be noted that these percentages are difficult to calculate precisely because the total number of cases remains unknown.
By contrast, the aforementioned MERS virus has got an estimated mortality rate of 35 percent, and the bird flu H5N1 a staggering 60 percent. Considering the sheer number of conspiracy theories out there and some people not accepting the science, I do feel the need to underscore the fact that COVID-19 is not “just a flu”. Even though the number of infections does not approach those of the flu, which according to WHO estimates infects around 1 billion people a year, the risk of death is estimated to be about 3.5 times that of the flu. Nevertheless, the mortality rate is clearly not in the range of some other zoonotic diseases, so in a sense, we have been relatively lucky with COVID-19. This could of course change in the future, if the virus keeps mutating like it does now, but more on that later.
How we are contributing to the rise of pandemics
As I mentioned at the beginning of this article, we are making pandemics more likely through our behaviour. The image below shows a breakdown of the drivers of disease emergence over the past century. A few of these I will now further expand on, because I believe that they are highly indicative of how the way we treat the planet contributes, among many other things, to the rise of disease.

Changes in land use single biggest driver of diseases
The above figure quite clearly shows that “land use changes” are the biggest driver of disease outbreaks. A study that was published in Nature last year found that animals that carry pathogens that are known to infect humans are more common in landscapes that have been altered. One of the main ways in which humans change the environment is through deforestation, with nearly 2-3% of global (tropical) forest cover still lost each year. This brings wildlife and humans in closer contact with each other, increasing the likelihood for both zoonotic and vector-borne diseases (recap: diseases caused by parasites, bacteria, or viruses). For instance, a study into forest loss in the Amazon found a connection between deforestation and malaria incidence. The rise of oil palm plantations has also been linked to outbreaks of other vector-borne diseases. Interestingly, transmission of zoonotic diseases “from wildlife directly to humans is uncommon”. This is where domestic animals come in, they can “bridge the gap.”
Deforestation also leads to the reduction and fragmentation of the habitats that species live in. This causes more interactions between the different species. Another consequence is the dying out of predators, who no longer have enough prey in the fragmented patches of land that remain, which means that the species that they hunted start increasing in numbers. This decreases the biodiversity of the area and makes disease outbreaks more likely. A study into Lyme disease (another vector-borne disease, transmitted through tick bites) found a “dramatic reduction” in the number of ticks carrying the disease in areas where biodiversity was higher. This means that in areas with a low biodiversity, which is usually the case in areas that humans have altered, the risk of getting Lyme disease from a tick is higher.
Furthermore, there are also many complex consequences of land use change that are easy to overlook, unless you happen to be directly affected by it, like the effect of mining, which often leads to the release of toxic chemicals into the environment. One example is mercury, which is released during gold mining and because of deforestation (through the erosion of the mercury-rich soil). Mercury accumulates in local fish populations, and in this manner finds its way into our bodies. In high doses this can be fatal, but even in lower doses this substance lowers our immune system and makes us more susceptible to disease.
Factory farms are not only breeding grounds for animals
On factory farms, animals like chickens and pigs are often crammed together in small, confined spaces for extended periods of time. Because these animals are solely bred for their meat or the products that they produce, the genetic diversity in these large groups of animals is low and side-effects of this breeding process include heart failure, cancer, and the growth of “crippling and painful skeletal deformities”. Add to that the frankly horrific conditions that exist in way too many of these places, where thousands upon thousands of animals are forced to stand—because there is no room to sit or lay down – in their own urine, faeces, blood, and pus, as well the decaying remains of those that do not manage to survive. I probably do not have to explain that these conditions cause incalculable levels of stress. Each and every one of these factors makes them more susceptible to disease and makes diseases spread more quickly, which then necessitates massive cullings in order to contain it.
Even if we put aside the complete and utter absence of an ethical or moral way of treating other living beings whose intelligence is higher than most people are aware of, it is hard to fathom conditions that are more suitable for disease outbreaks. To counteract the recurrent outbreaks – without reducing the number of animals or improving their living conditions – they are routinely fed antibiotics to keep them alive, with around eighty percent of all antibiotics going to factory farms. Because pathogens continually adapt to their environments, this widespread use of antibiotics invariably results in diseases that are resistant to them. That is why it would be prudent to use them sparingly, so that they remain useful as long as possible. Just to give an idea of how serious this problem of antibiotic resistance already is: in the U.S., a person dies every fifteen minutes because of “an infection that antibiotics can no longer treat effectively”.
In summary, the current way in which domestic animals are treated make disease outbreaks more likely, and when they do break out they might very well be resistant to antibiotics. This not only can lead to full-scale pandemics with all the loss of life and economic damage that comes along with it, but also means that millions of farm animals will be killed en masse, either to prevent further spread of the disease or because they can no longer be sold. The COVID-19 virus may not have originated in a factory farm, but previous pandemics have. A recent example is the 2009 swine flu (H1N1) mentioned earlier, which is thought to have first circulated among pigs. Two or more of these influenza strains then combined into a new strain with gene segments from humans, birds, and pigs, using the pigs as a “mixing vessel”. It is through this same mechanism that zoonotic diseases from wildlife often find their way to us.
The changes in our biosphere to come
Then there is the elephant that can be found in just about every room on Earth these days: climate change. Climate change acts as a threat multiplier to just about every threat we face, from tornadoes and hurricanes to hunger and disease. Just like how smoking cigarettes makes you more susceptible to just about any disease, including a heightened risk of severe COVID-19, so too does climate change make events that are bad enough on their own much, much worse. Disease outbreaks are no exception. The changing climate affects environments, changing which species can survive where. As environments change, some species might proliferate, like the tropical mosquitoes that are increasingly found in Northern regions, whereas others will be forced to move to other areas. The latter situation also applies to humans, mind you, as the current record number of 80 million refugees, roughly 1% of humanity, could rise as high as 1.2 billion in 2050. These two factors combined will increase the risk of disease transmission, the speed with which it will spread, and make containing it and addressing the underlying causes even more difficult.
Where do we go from here?
In conclusion, humans help make disease outbreaks more likely. Mainly by changing environments, through deforestation, agriculture, and climate change, and by keeping large numbers of genetically similar animals together in conditions that can best be summarised as ‘pathogen paradise.’ Our globalised society ensures that once a disease manages to jump to humans, it can spread around the world in a matter of days. Once a virus goes global, the only way to combat it is to contain its spread as much as possible and vaccinate everyone. So where do we go from here?
The short-term solution: Vaccine access
The People's Vaccine Alliance recently estimated that at current rates, it will take 57 years to fully vaccinate low-income countries. Conservative estimates of the excess doses procured by the U.S., E.U., U.K., Australia, Canada, and Japan are at over 1 billion. This means that these countries “could share over 1 billion doses of leading COVID-19 vaccines with other countries and still retain enough supply to inoculate their entire populations.”
To get a better understanding of the problems with vaccine access, I spoke to Tayyiaba Farooq, who is the project manager of the Free the Vaccine Campaign, an international collective of volunteers who are making the case for making vaccines available for everyone. “The main issue in such a disparity in vaccine access is due to the fact that lower and middle-income countries (LMICs) are effectively stocked out getting access to a supply.” she explained to me. “Since higher-income countries have bought up all of the vaccine supply, LMICs are left last in line to get access to the vaccines. This is due to the fact that many of these countries are able to afford to buy up large supplies of vaccine stock, a capability that many countries do not have. This leaves LMICs relying on alternative vaccines, and global aid through forms such as COVAX that still end up falling short of need.”
Government officials from Western countries state that the best way to get vaccines to the Global South in the current economic system is buying them up and consequently donating or lending them. This is perhaps best exemplified by the Biden administration’s recent announcement to donate 500 million vaccine doses. According to Farooq, the issue with such attitudes is that they rely on the assumption that the virus will pause in anticipation for vaccine deliveries. “But the reality is that while LMICs wait for the vaccine, the pandemic rages on, claiming lives, draining these countries of their resources, and giving the virus a chance to mutate, which has happened in places like India, South Africa, and the UK. Prolonging the pandemic does not help anyone and opens the possibility of making current vaccines less effective.”
In addition to the wealth disparities that seem to be at the heart of the unequal distribution of vaccines, countries face another major obstacle to getting access. Ever since the first vaccines became available, over one-hundred countries from the Global South have been pushing for a temporary waiving of intellectual property rights, with fierce opposition from Western countries. In fact, there many other factories, in countries like Bangladesh and South-Africa, that could be producing vaccines right now but lack the “blueprints and technical know-how”. Personally, I struggle to find any other justification for preventing other companies and countries from producing and distributing vaccines, except to ensure that even more billions of dollars of profit for pharmaceutical giants and their shareholders, for vaccines which could not have been developed without billions of dollars of funding from governments the world over, not to mention the fact that the countries that helped develop the vaccine often lack access to it.
Last month, President Biden threw his support behind waiving intellectual property protections for COVID-19 vaccines – referred to as a TRIPS waiver – but other Western countries remain opposed or pushing for facilitating ‘voluntary licensing agreements’ with pharmaceutical companies. The U.S.’ support for the TRIPS waiver is consequential, says Farooq, because it serves as a signal to for the rest of the world to move into this direction. “Accessibility to COVID-19 technology is essential in ensuring that LMICS can rely on alternative methods of sourcing COVID vaccines and treatments. By releasing the IP related to such health technologies, local manufacturers can start building up supplies for local municipalities. It also helps to make the supply chain associated with maintaining the vaccine’s integrity strong. Both the Moderna and Pfizer (along with others) vaccines must be kept at refrigerated temperatures to prevent its expiration. This cold chain supply is much easier to maintain when the vaccine is travelling domestically, as compared to receiving vaccine supplies from halfway across the world.” According to Farooq, the temporary waiving of IP protections would allow for a sustainable solution in effective worldwide distribution, which will undermine “the assumption that LMICs are not able to help themselves and must rely on the developed world for their salvation.”
In conclusion, solving the issues around vaccine access would go a long way towards improving the current situation. This will prevent many of the deaths and quality of life losses due to COVID’s pernicious aftermath, as well as the mutations that might make vaccines less effective. The consequences of COVID with the mortality rate of a swine flu are, frankly, too terrible to imagine. It is therefore not only immoral, but also against our own self-interest, to allow such an inequitable distribution of vaccines to persist. Instead of vaccines going to the world’s richest countries, who have bought enough vaccines to vaccinate their countries many times over, it would be a better idea to ensure equal vaccine access, and to prioritise regions with the highest disease prevalence and transmissions levels in order to reduce the risk of new variants emerging.
The long-term solutions
But then there is the longer term. As the many studies and examples discussed in this article show, we are almost guaranteed to be dealing with another major outbreak in the not too distant future, unless we address the drivers of disease outbreak that we are amplifying.
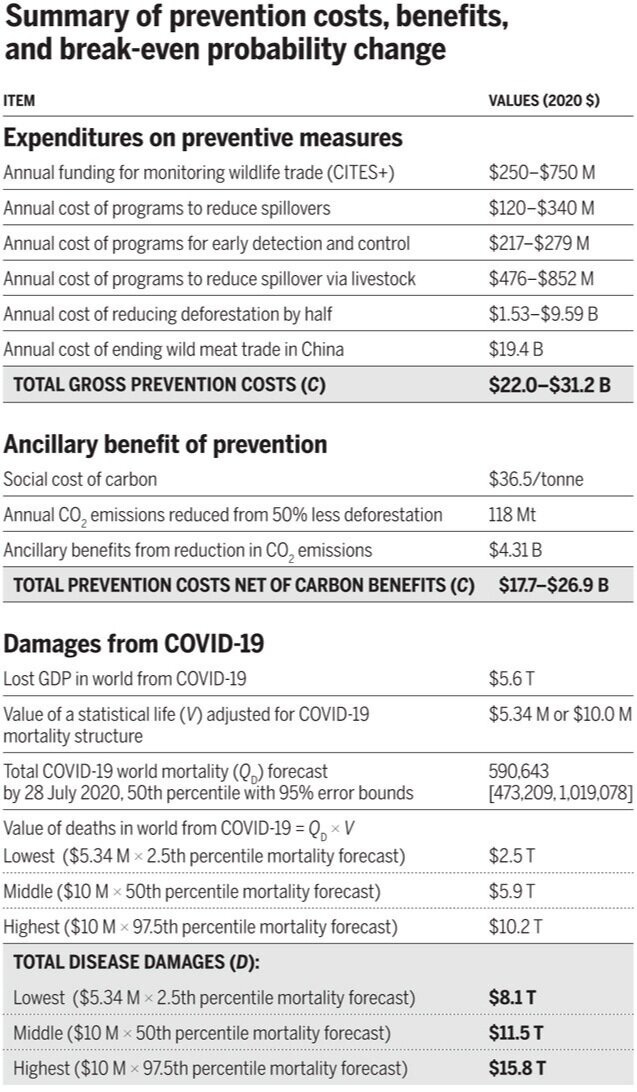
First, there is the issue of early detection and transparency. COVID-19 was allowed to spread for over forty days while the Chinese government tried to cover up information about the disease. Ensuring transparency and investing in the surveillance of emerging diseases are both crucial in containing outbreaks and ensuring that they do not rise to the scale of a pandemic. Surveillance and prevention bring with it significant initial costs, but these costs are outweighed by the gains to society, the agricultural sector, and wildlife, not to mention the public health benefits. Just to put some numbers on it, a study published in Science made an estimative summary of what these yearly disease prevention costs and benefits would look like, and compared it to the total damages (expected to be) inflicted by COVID-19, see the image below.
Second, there is the preparation and response to the pandemic. It should come as no surprise that health care – and other ‘essential’ fields like education for that matter – were already underfunded way before the pandemic. Years of austerity measures and spending cuts have resulted in weakened and often privatised health care systems, with too little staff, hospital beds, and vital equipment. Especially gruelling is the fact that public health workers are underpaid and overworked. Since 2014, the number of public health workers that plans to leave their job has gone up by 41%.
Despite the constant warnings the past decades that “significant change was needed, the majority of recommendations were never implemented”, concluded an independent panel this year. In the 86-page report, the panel claims that the pandemic was “preventable”, “due to a myriad of failures, gaps and delays in preparedness and response” and a “failure to learn from the past”, and laments that health threats have not been treated with the same vigour as “threats of war, terrorism, nuclear disaster or global economic instability.” As unprepared health care systems struggled to cope with the surges in patients, often at the expense of other essential health services, they were held together by health professionals and other essential workers. They worked “hour after hour, often lacking adequate protective equipment and patient supplies, watching helplessly while patients died without loved ones by their sides, and worrying about their own health and families.” Furthermore, supplies of medical equipment, testing materials, and things like masks, were overly dependent on a few manufacturers and countries, and resulted in “hoarding, price-gouging and fraud”.
Some of the solutions that the panel proposes are:
A global health threats council to ensure better communication and coordination between countries
An international system with accessible and sufficient stockpiles
A stronger and more authoritative role World Health Organisation
Investing in the earlier mentioned global preparedness and epidemic surveillance
Third, reducing deforestation is one important way to reduce the odds of pathogens spreading from animals to humans. The aforementioned study into prevention costs and benefits found that “the clear link between deforestation and virus emergence suggests that a major effort to retain intact forest cover would have a large return on investment even if its only benefit was to reduce virus emergence events.” This does not have to come at a large economic cost. For instance, between 2005 and 2012, Brazil reduced deforestation by 70%, even though soy crop production increased. Planting trees also has the added benefit of improving biodiversity and could make a significant contribution towards slowing down global warming.
Fourth, the way in which our society treats farm animals like disposable commodities significantly contributes to the spread of diseases and the emergence of new ones. If we are serious about reducing this risk, serious changes have to be made to the way in which meat is produced and consumed. Basically, we have to eat less meat, which is incidentally also essential for realistically meeting climate goals, and simultaneously we have to find ways to massively reduce the scale and methods used to keep domestic farms animals, so that there is no need for massive deployment of antibiotics just to keep these genetically similar masses of highly weakened and confused animals alive long enough for harvesting.
Lastly, there is the overarching problem of our unfolding climate and biodiversity crisis. As environments change and ecosystems are even further disturbed than they already are, animals and people will be forced to move due to food shortages, droughts, floods, hurricanes, and other factors that will make living in many areas impossible. In addition to the movement of so many different species, there will also be certain species that are able to take advantage of the new environments. The expansion of malaria-carrying mosquito populations towards Europe is a clear example of this. The calls for solidarity in the fight against COVID-19 in the run-up to this month’s G7 summit have been accompanied by ominous warnings that a failure to address this global crisis in an equitable and just way is likely to seriously hamper the chances of success of this year’s climate summit (COP26). Not something that we can afford when we are, in the words of the UN’s Secretary-General, on “the verge of the abyss”.
To be honest, after going into such depth about the COVID-crisis and its root causes, I do not think that I have the words to properly convey to you how precarious our current moment in history is. In the latest episode of my (Dutch) podcast ‘de Vragenboom’, I explored the question of how to act in the face of imminent climate catastrophe when we might already be past the point of no return. I strongly encourage my Dutch audience to go listen to it, but for the rest of you I shall summarise the conclusion that I reached. I still feel that I must do everything I can, not only because it is the right thing to do and the alternative is fatalistic despair, but because I cannot live with myself if I did anything less. I am not going to tell you that you need to do the same, because this is something that everyone needs to figure out for themselves. But whatever your own answer to that question might be, make sure that you can live with it.
Note: This post was first published on www.criticalconsent.com